This study abides by the Declaration of Helsinki of ethical standards and is also approved by the Ethics Committee of the Isfahan University of Medical Sciences. In this study, we evaluated the long-term efficacy of the CXL to stabilize vision, refraction, and topography in PMD after 5 years of follow-up. CXL, whenever proved to be effective in halting or slowing down the progression of PMD, can lessen the need for more aggressive and complex surgeries with a high risk for complications. 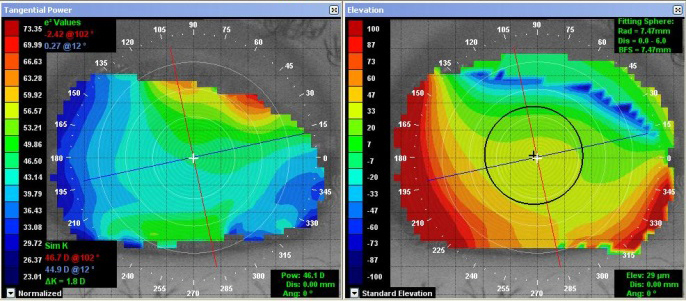
have noted the need for long-term evaluation of CXL on PMD in their reviews. , Sorkin and Varssano and Jinabhai et al. ,, ,, Few studies with a more extensive scope have only evaluated patients after a short-term follow-up. 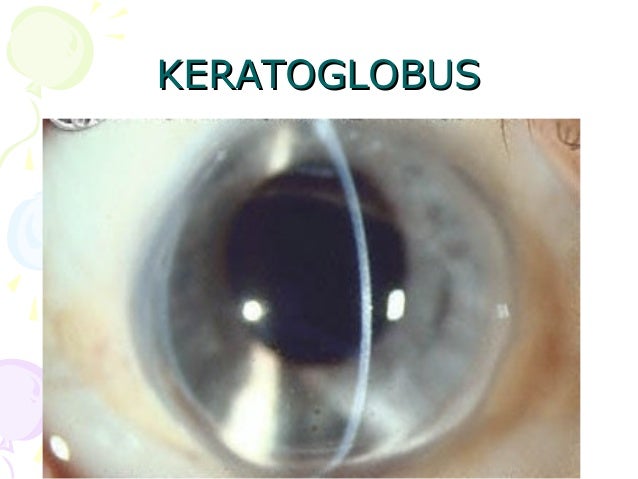
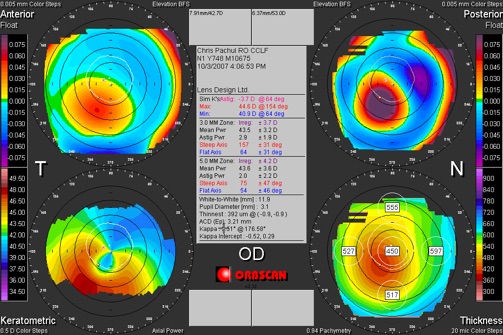
There have been studies centered on the use of CXL in PMD patients, but most of these studies are case reports. And is one of the most popular methods for treating patients diagnosed with keratoconus. Ĭorneal cross-linking (CXL) is a technique that can halt the progression of keratoconus. Surgical methods consist of intrastromal corneal ring segment, penetrating keratoplasty,, lamellar crescentic keratoplasty,, and more novel methods such as sliding keratoplasty. Surgical methods are often used in patients with advanced progressive disease or cases that cannot use contact lenses. and other researchers, recommended toric soft contact lenses for high irregular astigmatism. concluded that patients with high degrees of astigmatism using spherocylindrical glasses with high refraction indices, had acceptable visual acuity. Nonsurgical methods used to treat PMD are glasses and gas permeable hard contact lenses. The current treatment plans for PMD consist of nonsurgical and surgical methods. Currently, there is no evidence of PMD being a hereditary disease, but studies have discussed that moderate-to-severe astigmatism is observed in the immediate relatives of PMD patients. Studies show that PMD is observed in all races and is not confined to a specific geographical region. PMD is mostly diagnosed between the second and fifth decades of life. These findings were in agreement with prior studies. in 2004, including 116 eyes from 58 patients, 77.6% of patients were male. According to one of the large-scale studies on PMD, published by Sridhar et al. There is no known etiology for PMD yet, and no unanimous consensus whether PMD, keratoconus, and keratoglobus are distinct diseases or just different phenotypes of the same disorder. ,, Schlaeppi noticed the absence of lipid deposition, scarring, or vascularization in PMD, the so-called pellucid. , PMD manifests as impaired vision due to high against the rule and irregular astigmatism with a characteristic butterfly appearance or crab-claw pattern in corneal topography. The disease mainly affects the inferior and peripheral portions of the cornea. Pellucid marginal degeneration (PMD), initially described by Krachmer in 1978, is a bilateral noninflammatory progressive corneal ectatic disorder. Corneal cross-linking in pellucid marginal degeneration: Evaluation after five years. How to cite this URL: Irajpour M, Noorshargh P, Peyman A. How to cite this article: Irajpour M, Noorshargh P, Peyman A. Keywords: Corneal cross-linking, Corneal ectasia, Pellucid marginal degeneration Furthermore, regarding steep keratometry values, 25 subjects were stable, 7 had improvements, and 8 worsened.Ĭonclusion: CXL appears to be a safe and effective procedure to halt the progression of PMD. The spherical equivalent refractive error improved in 4 subjects, was stable in 25, and worsened in 11 subjects, while a 0.5 diopter or more myopic change was considered significant. Regarding the BCVA Snellen lines, 23 eyes had no significant change in pre- and postoperative examinations, 11 eyes had improvement, and 6 subjects showed worsening defined as significant when two or more lines change. We did not find any significant difference between pre- and postoperative spherical equivalent and spherical refractive errors ( P = 0.419 and P = 0.396, respectively). No statistically significant difference was noted comparing preoperative mean logMAR best-corrected visual acuity (BCVA) and postoperative mean logMAR BCVA (0.24 ± 0.19 and 0.22 ± 0.20, P > 0.05). Results: The comparison between mean preoperative logMAR uncorrected visual acuity and 5-year postoperative evaluation revealed no significant change (1.20 ± 0.65 and 1.17 ± 0.64, P > 0.05). Visual acuity, refraction, and topography data were compared to their respective values before CXL. All subjects had undergone CXL for PMD at least 5 years before the assessments. Methods: In a retrospective study, forty eyes of forty patients were enrolled. Purpose: To evaluate the long-term outcome of corneal cross-linking (CXL) for pellucid marginal degeneration (PMD). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
